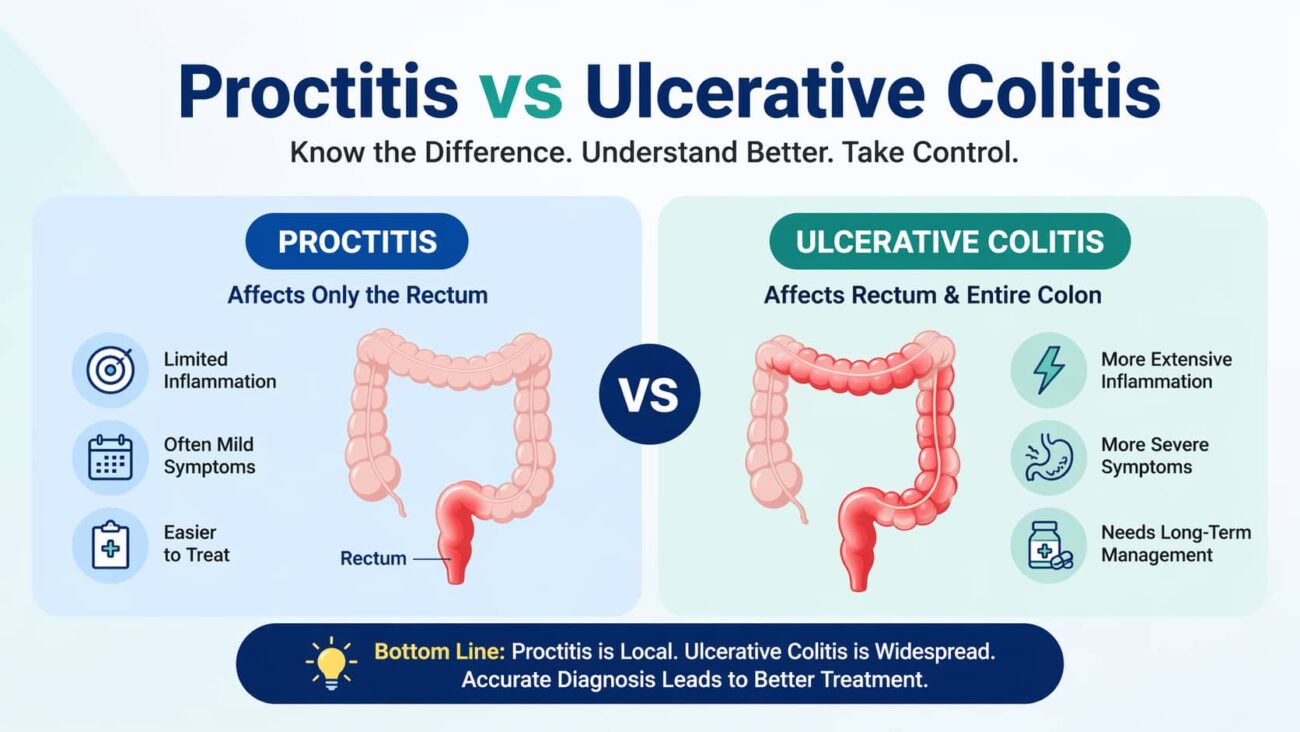
Proctitis vs Ulcerative Colitis: Key Differences, Symptoms & Treatments Explained
You’re dealing with rectal bleeding, urgent bathroom trips, and that relentless cramping that won’t let you live normally. Your doctor throws out two terms — proctitis and ulcerative colitis — and suddenly you’re more confused than before.
They sound similar. They share some symptoms. They both involve bowel inflammation. But they are not the same condition — and treating them as if they were is a mistake that can cost you years of ineffective care.
This guide breaks down proctitis vs ulcerative colitis in plain language: what each condition is, how they differ, why it matters for your treatment, and exactly what you can do about it.
Proctitis vs ulcerative colitis: Proctitis is inflammation confined to the last 6 inches of the rectum. Ulcerative colitis is a chronic inflammatory bowel disease that can affect the entire colon. Proctitis is often milder and easier to treat, while ulcerative colitis carries a higher risk of complications and may require long-term systemic therapy.
What Is Proctitis?
Proctitis is inflammation of the rectal lining — the innermost 15–20 centimeters (roughly 6 inches) of the large intestine. It does not extend further up into the colon.
The condition can be acute (sudden onset) or chronic (ongoing for weeks to months), and its severity ranges from mild irritation to ulcerated, bleeding rectal tissue.
What Causes Proctitis?
Proctitis is not a single disease — it’s a pattern of inflammation with multiple possible causes:
- Sexually transmitted infections (STIs): Gonorrhea, chlamydia, herpes simplex virus, and syphilis are among the most common infectious causes, particularly in sexually active individuals.
- Inflammatory bowel disease (IBD): Ulcerative colitis or Crohn’s disease limited to the rectum can present as proctitis.
- Radiation therapy: Pelvic radiation for prostate, cervical, or rectal cancer can damage the rectal lining — this is called radiation proctitis.
- Antibiotics: Antibiotic use can disrupt gut flora and trigger Clostridioides difficile-related proctitis.
- Autoimmune or idiopathic causes: In some cases, no specific trigger is found.
Who Gets Proctitis?
Proctitis can affect anyone, but certain groups carry higher risk: men who have sex with men (due to STI transmission routes), cancer patients undergoing pelvic radiation, people with IBD, and individuals who have recently taken broad-spectrum antibiotics.
What Is Ulcerative Colitis?
Ulcerative colitis (UC) is a chronic inflammatory bowel disease that causes persistent inflammation and ulcers in the lining of the colon and rectum. Unlike proctitis, UC is a systemic, autoimmune-mediated condition that follows a relapsing-remitting course — meaning symptoms flare up and then settle, often unpredictably.
UC almost always starts in the rectum and can spread continuously up through the colon. In some people, the inflammation remains limited. In others, it extends to involve the entire colon — a condition called pancolitis.
What Causes Ulcerative Colitis?
The exact cause remains under investigation, but research points to a combination of:
- Immune system dysregulation: The immune system mistakenly attacks the colon’s mucosal lining, triggering chronic inflammation.
- Genetic predisposition: Having a first-degree relative with UC significantly increases your risk. Over 200 genetic loci have been linked to IBD.
- Gut microbiome imbalance: Disruption in the balance of intestinal bacteria (dysbiosis) is strongly associated with UC flares.
- Environmental triggers: Diet, smoking cessation, NSAIDs, and psychological stress can all trigger or worsen symptoms.
Who Gets Ulcerative Colitis?
UC affects roughly 1 in 200 people in Western countries. It typically first appears between ages 15–35, though it can develop at any age. It affects men and women roughly equally. Rates are rising in developing nations, likely linked to Westernized diets and lifestyle changes.
Proctitis vs Ulcerative Colitis: Side-by-Side Comparison
| Feature | Proctitis | Ulcerative Colitis |
|---|---|---|
| Location of inflammation | Rectum only (last 15–20 cm) | Rectum + part or all of colon |
| Disease type | Can be infectious, radiation-related, or IBD-related | Chronic autoimmune IBD |
| Rectal bleeding | Common | Common (often with mucus) |
| Diarrhea | Mild or absent — may have constipation | Frequent, often bloody diarrhea |
| Abdominal pain | Usually mild, localized to lower rectum | Cramping, can be severe and widespread |
| Systemic symptoms | Rare (unless systemic infection) | Fatigue, weight loss, fever, joint pain |
| Colonoscopy appearance | Inflammation confined to rectum | Continuous inflammation extending into colon |
| Cancer risk | Low (unless IBD-related) | Elevated after 8–10 years, especially pancolitis |
| Treatment scope | Topical (suppositories, enemas) often sufficient | Often requires oral or systemic medications |
| Prognosis | Good; often resolves with appropriate treatment | Chronic; requires ongoing management |
Symptoms of Proctitis vs Ulcerative Colitis
Symptoms of Proctitis
Because the inflammation is restricted to the rectum, many symptoms are localized:
- Rectal bleeding — bright red blood on toilet paper or in the toilet bowl
- Rectal pain, pressure, or a persistent feeling of needing to pass stool (tenesmus)
- Passing small amounts of mucus or blood without stool
- Anal discomfort or pain during bowel movements
- Paradoxically, constipation is common — unlike UC, where diarrhea dominates
- In infectious proctitis: discharge, fever, or genital sores may also appear
Symptoms of Ulcerative Colitis
UC symptoms tend to be more widespread and include systemic features:
- Frequent, urgent, bloody diarrhea — sometimes 6–10+ times per day during flares
- Abdominal cramping and pain — often worse before bowel movements
- Rectal urgency and tenesmus
- Fatigue and general weakness
- Unintentional weight loss
- Low-grade fever during active flares
- Anemia from chronic blood loss
- Extra-intestinal symptoms: joint pain (arthropathy), skin rashes (erythema nodosum), eye inflammation (uveitis), and liver involvement (primary sclerosing cholangitis)
How Are They Diagnosed?
Accurate diagnosis is critical — the treatment for infectious proctitis is completely different from the treatment for UC. Getting this wrong means months of ineffective therapy.
Diagnosing Proctitis
A gastroenterologist will typically use:
- Sigmoidoscopy or colonoscopy: The definitive test. A small camera examines the rectum and confirms that inflammation does not extend further into the colon.
- Biopsy: Tissue samples taken during the scope can confirm inflammation type and rule out cancer.
- STI testing: Swabs for gonorrhea, chlamydia, herpes, and syphilis are standard for suspected infectious proctitis.
- Stool cultures: To identify bacterial or parasitic causes.
Diagnosing Ulcerative Colitis
- Full colonoscopy with biopsy: The gold standard. Reveals continuous mucosal inflammation from the rectum upward, and distinguishes UC from Crohn’s disease.
- Blood tests: Checking for anemia, elevated inflammatory markers (CRP, ESR), and nutritional deficiencies.
- Fecal calprotectin: A stool test that measures intestinal inflammation — useful for monitoring disease activity and ruling out irritable bowel syndrome (IBS).
- Imaging (CT/MRI): Used in severe or complicated cases to assess complications like toxic megacolon.
Treatment: Proctitis vs Ulcerative Colitis
This is where the two conditions diverge most dramatically. Understanding the treatment difference is one of the most practical reasons to get an accurate diagnosis.
Treating Proctitis
Treatment depends entirely on the underlying cause:
Infectious proctitis:
- Gonorrhea/chlamydia: Treated with antibiotics — typically ceftriaxone plus doxycycline.
- Herpes proctitis: Antiviral medications such as acyclovir reduce duration and severity.
- Syphilitic proctitis: Treated with penicillin G.
IBD-related proctitis (ulcerative proctitis):
- Topical mesalazine (5-ASA) suppositories or enemas — first-line therapy with high success rates.
- Topical corticosteroids for short-term relief during flares.
- Oral mesalazine added when topical therapy alone is insufficient.
Radiation proctitis:
- Sucralfate enemas and anti-inflammatory agents are used.
- Argon plasma coagulation (APC) — an endoscopic procedure — can treat bleeding from radiation-damaged blood vessels.
Treating Ulcerative Colitis
UC treatment is stratified by disease extent and severity:
Mild to moderate UC:
- Oral 5-aminosalicylates (mesalazine, sulfasalazine) — the cornerstone of UC therapy for mild-moderate disease.
- Topical 5-ASA preparations used alongside oral therapy for left-sided or rectal involvement.
Moderate to severe UC:
- Corticosteroids (prednisone) for short-term induction of remission.
- Immunomodulators: azathioprine or 6-mercaptopurine for maintenance.
- Biologic therapies: anti-TNF agents (infliximab, adalimumab), vedolizumab (integrin inhibitor), or ustekinumab (IL-12/23 inhibitor) for moderate-to-severe refractory disease.
- JAK inhibitors (tofacitinib, upadacitinib): newer oral targeted therapies with rapid onset of action.
Surgery:
- Proctocolectomy (removal of colon and rectum) is considered curative for UC, used in medically refractory cases or when cancer risk becomes significant.
Can Proctitis Turn Into Ulcerative Colitis?
Yes — in some people, ulcerative proctitis (IBD confined to the rectum) can spread to involve more of the colon over time, effectively progressing to ulcerative colitis. Studies suggest that approximately 10–30% of patients with ulcerative proctitis experience proximal extension within 10 years. Regular monitoring with colonoscopy is essential.
This is one of the most important clinical points in the proctitis vs ulcerative colitis discussion. A person diagnosed with isolated proctitis may not have UC today — but without adequate treatment and monitoring, they could develop more extensive disease later.
Factors associated with higher risk of extension include: inadequate response to initial treatment, persistent mucosal inflammation, and higher levels of fecal calprotectin at diagnosis.
The Role of the Gut Microbiome in Both Conditions
Both proctitis and ulcerative colitis are increasingly understood through the lens of gut health. The composition of your intestinal microbiome — the trillions of bacteria living in your colon — plays a central role in regulating mucosal immunity.
In UC, research consistently shows reduced microbial diversity and a decreased abundance of protective bacteria such as Faecalibacterium prausnitzii and Roseburia hominis, both known for their anti-inflammatory short-chain fatty acid production.
Dysbiosis (microbiome imbalance) can also worsen inflammatory proctitis and slow recovery. Supporting your gut microbiome through diet, managing antibiotic use wisely, and considering evidence-based probiotic supplementation are all reasonable adjunct strategies — though they are not a substitute for prescribed medical treatment.
If you’re managing any form of gut inflammation, understanding the wider landscape of gut health is critical. Our guide on probiotic side effects is a helpful read before starting any supplement protocol. And if irritable bowel symptoms overlap with your presentation, our evidence-based overview of the best probiotics for IBS is worth exploring.
Diet, Lifestyle, and Managing Flares
What to Eat During a Flare
There is no universal “IBD diet,” but clinical experience and patient data point to some consistent patterns:
- Low-residue diet: During active flares, reducing fiber temporarily (white rice, cooked vegetables, low-fat proteins) can ease stool frequency and rectal urgency.
- Avoid trigger foods: Common culprits include spicy foods, alcohol, carbonated drinks, high-fat fried foods, and raw vegetables with tough skins.
- Stay hydrated: Frequent stools lead to fluid and electrolyte loss — prioritize water, diluted coconut water, or oral rehydration solutions.
- Small, frequent meals: Reduces the gastrocolic reflex that can trigger post-meal urgency.
Lifestyle Factors That Matter
- Stress management: The gut-brain axis is real. Chronic stress activates inflammatory pathways and is a documented trigger for UC flares. Mindfulness, yoga, and cognitive behavioral therapy (CBT) have evidence behind them for IBD symptom management.
- Exercise: Regular moderate exercise (walking, cycling, swimming) supports gut motility, reduces inflammation, and improves mental health outcomes in IBD patients.
- Sleep: Poor sleep quality independently predicts UC flare severity. Aim for 7–9 hours consistently.
- Smoking: Paradoxically, smoking appears slightly protective against UC but worsens Crohn’s disease. Quitting smoking can occasionally trigger a UC flare — discuss this with your doctor before making changes.
If bloating and digestive discomfort are part of your picture, our comprehensive guide on the best probiotics for bloating covers which strains have the strongest clinical data for gut symptom relief.
Complications: What Happens If Left Untreated?
Untreated Proctitis
- Infectious proctitis that goes untreated can lead to fistulas (abnormal channels between the rectum and surrounding tissues) or perianal abscesses.
- STI-related proctitis can spread systemically — untreated gonorrhea, for example, can cause disseminated infection affecting joints and heart valves.
- Chronic radiation proctitis may lead to severe rectal bleeding, stricture formation (narrowing of the rectum), and fistula development.
Untreated Ulcerative Colitis
- Toxic megacolon: A life-threatening dilation of the colon that requires emergency surgery.
- Colorectal cancer: The risk increases significantly after 8–10 years of extensive colitis — regular surveillance colonoscopy is standard care.
- Severe anemia and malnutrition: From chronic blood loss and nutrient malabsorption.
- Primary sclerosing cholangitis (PSC): A serious liver complication affecting 2–5% of UC patients that can progress to liver failure.
- Osteoporosis: Long-term corticosteroid use and malabsorption reduce bone mineral density.
Understanding the difference between proctitis and ulcerative colitis is about more than terminology — it’s about avoiding these serious downstream consequences through timely, targeted treatment.
For a broader look at the body’s inflammatory and autoimmune processes, our article on autoimmune hepatitis explains how the immune system can attack the body’s own tissues across different organ systems.
When to See a Doctor
Many people delay care out of embarrassment or because they assume rectal symptoms will resolve on their own. They often don’t.
See a doctor promptly if you experience:
- Rectal bleeding lasting more than a few days
- More than 4 loose or bloody stools per day
- Significant rectal pain that disrupts daily life
- Fever above 38°C (100.4°F) alongside bowel symptoms
- Unintentional weight loss of more than 2–3 kg over weeks
- Rectal symptoms following recent sexual activity — especially unprotected anal sex
- Symptoms that do not improve within 2–4 weeks of starting treatment
Ask to be referred to a gastroenterologist — a specialist in digestive diseases — rather than relying solely on a general practitioner for ongoing inflammatory bowel symptoms. A specialist-led care model significantly improves long-term outcomes in both proctitis and UC.
For authoritative clinical guidance, the Crohn’s & Colitis Foundation provides extensive patient resources, clinical trial information, and specialist directories. Additionally, the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) publishes regularly updated, peer-reviewed information on UC diagnosis and treatment.
A Note on Probiotics and Gut Support
While probiotics are not a treatment for either proctitis or ulcerative colitis, they can play a supportive role. Certain strains — particularly Lactobacillus and Bifidobacterium species — have shown modest benefits in maintaining UC remission and reducing the frequency of minor digestive complaints.
The key is choosing the right strain for the right purpose. Before adding any supplement to an IBD management plan, read our evidence-based overview of probiotics vs prebiotics to understand what each actually does in the gut — and which one makes sense for your situation.
Frequently Asked Questions
Conclusion: Why Getting the Diagnosis Right Matters
The distinction between proctitis vs ulcerative colitis is not just semantic — it determines your entire treatment plan, your long-term risk profile, and how aggressively your condition needs to be managed.
Proctitis, particularly when caused by infection, can be fully resolved. Ulcerative colitis is a lifelong condition that demands sustained care, regular monitoring, and often escalating medical therapy. Even when the two conditions share symptoms, the path forward is very different.
The most important thing you can do is push for a proper diagnosis: colonoscopy, biopsy, and appropriate testing rather than guesswork. Work with a gastroenterologist. Ask questions. And don’t accept vague answers when your bowel health is on the line.
This article is for informational purposes only and does not constitute medical advice. Always consult a licensed healthcare professional before making changes to your treatment plan. See our full medical disclaimer.